Bredesen-Protocol Strategies to improve brain health and reverse cognitive decline

At proactive wellness, we believe that there is no more important component of your overall health than brain health. Yet, before much of the emerging research that is being presented today, not much has been known about how to promote brain health and in particular how to lower risk for dementia/alzheimer’s and how to stabilize it for patients that already have early signs and symptoms through effective dementia treatment. At Proactive Wellness Centers, Dr. Lawson is one of the elite Bredesen Protocol practitioners, ReCode 2.0 Certified, with 17 years of functional medicine experience to get to the root cause of the cognitive decline of you or your loved one.
Keep reading to learn more about our exciting new Brain Health Optimization Program (BHOP), but before we go there, let’s understand a little background and relevant history.
For perspective, according to the CDC, Alzheimer’s disease (AD) is present in 50% of patients in nursing homes, causes more than 110,000 deaths in the US per year and was the 6th leading cause of death overall based on 2015 data. AD affects over 5 million people in the US alone. Some recent data suggests that the problem is getting worse based on early data from 2016 and 2017.
If we look beyond the United States, dementia is fast becoming one of the world’s most burdensome illnesses. According to the World Health Organization (WHO), there are currently around 47 million people across the globe living with dementia, and this number is expected to reach 75 million by 2030, and 132 million by 2050. AD is the most common form of dementia, accounting for around 60 to 80 percent of all cases.
Alzheimers Disease Symptoms
| Alzheimer’s disease Symptoms | Normal Aging |
| Memory loss that disrupts daily life, especially forgetting newly learned information | Forgetting newly learned information such as appointments or names but being able to recall them later |
| Having difficulty solving everyday problems such as paying bills | Making occasional errors but none that are significant or out of the ordinary |
| Struggling to complete familiar tasks such as driving home or to work | Needing help setting up new equipment or electronics |
| Losing track of dates, seasons, or time | Temporarily forgetting the day but having the ability to recall it laterTingling |
| Difficulty judging distance, spatial relationships, and contrast | Worsening vision caused by cataracts |
| Trouble recalling words for things, following conversations, and speaking | Shortness of breath |
| Misplacing items and not being able to retrace steps | Unusual pain |
| Poor judgement or decision-making; inability to multitask | Confusion |
| Social withdrawal | Difficulty regulating body temperature |
| Changes in personality and mood | Becoming irritated when things are not done a particular and preferred way. |
[dms-accordion]
Take our quick assessment. Or, if you are a concerned observer, answer from your observations of their behavior. If you or the observed person have more than 1 of the listed symptoms above, a cognitive evaluation is in order.
Signs and symptoms of AD are not normal signs of aging. If you or someone you love is experiencing any of these symptoms, it is important to make an appointment as possible because AD worsens over time.
AD is a progressive disease and although there is no cure, the Bredesen’s protocol has been able to slow and reverse cognitive decline. Remember, the earlier AD is caught, the easier it is to successfully treat the condition.
Once a person has noticeable symptoms, they are in the later stages of cognitive decline. AD has an initial “silent phase,” where brain degeneration is occurring but these changes are not detectable using objective tests. Patients may, however, notice slight memory and cognitive changes. See the image below.
Click here to gain a better understanding of AD and dementia and how they differ from “general aging”
AD is a form of dementia as illustrated by the graphic below:
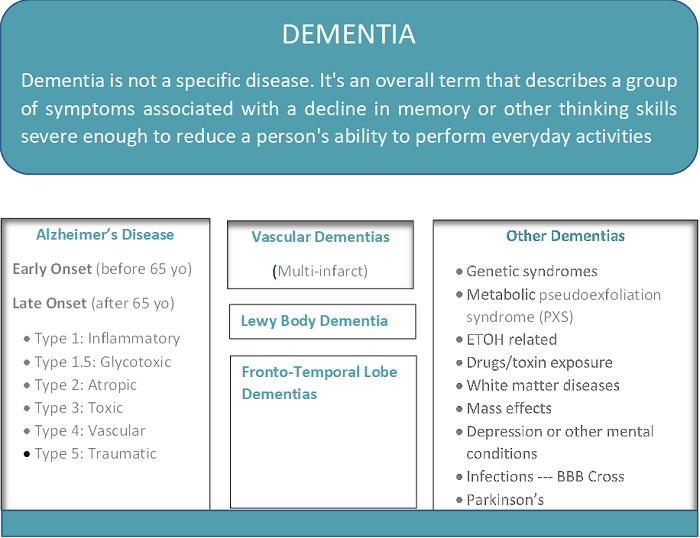
For understanding and to separate Alzheimer’s from “normal aging” it is helpful to define AD. Alzheimer’s disease (AD) is an irreversible (?), progressive brain disorder that slowly destroys memory and thinking skills and, eventually, the ability to carry out the simplest tasks. It is characterized by the development of amyloid plaques and neurofibrillary, or tau, tangles; the loss of connections between nerve cells (neurons) in the brain; and the death of these nerve cells. It is the most common cause of dementia in older adults. While dementia is more common as people grow older, it is not a normal part of aging. There are two types of Alzheimer’s—early-onset (very rare) and late-onset. Both types have a genetic component.
- Early-onset AZ is caused by any one of a number of different single-gene mutations on chromosomes 21, 14, and 1. Each of these mutations causes abnormal proteins to be formed. Mutations on chromosome 21 cause the formation of abnormal amyloid precursor protein (APP). A mutation on chromosome 14 causes abnormal presenilin 1 to be made, and a mutation on chromosome 1 leads to abnormal presenilin 2.
Each of these mutations plays a role in the breakdown of APP, a protein whose precise function is not yet fully understood. This breakdown is part of a process that generates harmful forms of amyloid plaques, a hallmark of the disease.
- Most people with Alzheimer’s have the late-onset form of the disease, in which symptoms become apparent in the mid-60s and later. The causes of late-onset Alzheimer’s are not yet completely understood, but they likely include a combination of genetic, environmental, and lifestyle factors that affect a person’s risk for developing the disease.
Researchers have not found a specific gene that directly causes the late-onset form of the disease. However, one genetic risk factor—having one form of the apolipoprotein E (APOE) gene on chromosome 19—does increase a person’s risk. APOE comes in several different forms, or alleles:
- APOE ε2 is relatively rare and may provide some protection against the disease. If Alzheimer’s disease occurs in a person with this allele, it usually develops later in life than it would in someone with the APOE ε4 gene.
- APOE ε3, the most common allele, is believed to play a neutral role in the disease—neither decreasing nor increasing risk.
- APOE ε4 increases risk for Alzheimer’s disease and is also associated with an earlier age of disease onset. A person has zero, one, or two APOE ε4 alleles. Having more APOE ε4 alleles increases the risk of developing Alzheimer’s.
- APOE ε4 is called a risk-factor gene because it increases a person’s risk of developing the disease. However, inheriting an APOE ε4 allele does not mean that a person will definitely develop Alzheimer’s. Some people with an APOE ε4 allele never get the disease, and others who develop Alzheimer’s do not have any APOE ε4 alleles.
Click here for a more complete understanding of APOE and its role in development of AD
Apolipoprotein E (apoE) has multiple roles, including lipid transport in the blood and the brain. The APOE4 variant increases the risk for late-onset Alzheimer’s disease and may contribute to the pathology of the disease through influence on β-amyloid, inflammation, or other processes.
The risk for development of late-onset AD is increased approximately two- to threefold for individuals with one copy of the APOE4 variant and by approximately 10- to 15-fold for individuals with two copies of the variant (E4/E4 genotype). The APOE2 variant has some protective effect against development of late-onset AD. The lifetime risk for late-onset Alzheimer’s disease is approximately 10% to 12% in the general population, though it is higher in women than men and doubles when there is a first-degree relative with this disorder. The lifetime risk is approximately 9% for individuals negative for APOE4, and for individuals with E4/E4 may be as high as 25% for males and 45% for females. Among patients with late-onset AD, the presence of APOE4 may lead to earlier development of symptoms.
What can a person do to minimize their risk for developing AZ and reverse cognitive decline?
Given that science has not yet established a specific causal factor, it is believed that the development of the disease is based on a combination of genetics (APOE), lifestyle factors, history of head trauma (ex. Athletes like football players), mitochondrial damage and toxin exposure including biotoxins (Mold exposure). From our functional medicine underpinning, we know that mitochondrial damage can be initiated by free radical damage and that this can be mitigated through effective detoxification, proper nutritional supplementation, ensuring gut health, healthy eating and other lifestyle factors. From our knowledge about the damage inflicted by CIRS (Chronic Inflammatory Response Syndrome from mold exposure) it is easy to conceptualize how CIRS is related to cognitive decline as may CIRS patients experience reversible cognitive decline if CIRS is left untreated.
After much research, Dr. Lawson determined that the Bredesen protocol provides the best evidenced-based approach to diagnosing and treating cognitive decline from AD and related illnesses. The world renowned Dr. Dale Bredesen has created the ReCODE protocol that involves multiple strategies to address specific health issues that contribute to Alzheimer’s Disease (AD). The results of each strategy are measured by using blood tests, cognitive evaluations, dementia tests, and other markers of overall health improvements. Dr. Lawson is now a Bredesen Certified doctor, ReCode 2.0 as she has completed the study and certification requirements to be able to offer patients the full Bredesen ReCODE protocol to help them recover from these debilitating illnesses. The only way to get this care is to see a Bredesen protocol doctor, Certified under ReCode 2.0 to ensure you are getting the best possible care.
At the forefront of this functional medicine approach to AD is Dr. Dale Bredesen and his team from the Buck Institute for Research on Aging. Through careful examination of the pathogenesis of Alzheimer’s, Doctor Bredesen and his team have found promising results. They have developed a multiple modality approach to achieving what they call metabolic enhancement for neurodegeneration (MEND), now referred to as Reversal of Cognitive Decline or Bredesen ReCODE.
Through the approach Doctor Bredesen has developed, patients have been able to dramatically improve cognitive function, achieve reversal of symptoms, and in some cases, return to work. The ReCODE program includes lifestyle interventions, therapeutic diets, and targeted nutrients. We are excited to add this promising Alzheimer’s disease treatment modality for the benefit of patients of Proactive Wellness Centers.
Baseline Bredesen Evaluation
We have two ways that we engage with patients seeking the Bredesen Protocol. First is our Baseline Bredesen Evaluation is suitable for patients that are asymptomatic — meaning that beyond the normal age-related decline, the patient does not have any meaningful cognitive decline. Dr. Bredesen refers to this scenario as a “PreCode” patient. Our Baseline Bredesen Evaluation is the starting point for PreCode patients or those that don’t know their status and risk factors. The baseline Evaluation includes all of the following:
- Baseline labs and physical examination. A very complete set of baseline labs that will evaluate the entire spectrum of health and a baseline physical examination closely following the Bredesen protocol. This goes well beyond standard labs to include magnesium, zine and selenium levels, B6, B12 and folate levels, Omega 3 and omega 6 fatty acid levels, pre-diabetes evaluation, hormone levels, thyroid levels as well as specific immune markers like TH1, TH2, IL6 and TNF. These labs are not included in our fee as they are billed to your insurance. For patients that do not have insurance or that have insurance that denies many labs, these baseline labs can be purchased from Apollo Health for the very reduced price of $780 plus the required Apollo membership at $75/month.
- A baseline Cognitive Assessment. This is to establish a baseline and evaluate you against an age-specific norm to determine the state of your cognitive function today. We are using the CNS Vital Signs cognitive assessment, one of the most highly regarded assessments in the industry. In addition, we will also perform the standard MoCA test as well.
- Apolipoprotein E (APOE) genetic test. This test is generally not covered by insurance but is an important component to our assessment. It will be included on the insurance panel. If in doubt about coverage, contact your insurance carrier directly.
- A physical examination.
- 2-hour consultation with our ReCode 2.0 Certified Physician. This will cover the review of the lab results and a detailed plan of action to address sub-optimal areas identified in the Evaluation.
The cost for the Bredesen Baseline Evaluation is $1975 and includes the components listed above.
Bredesen Complete Brain Health Optimization Program
For patients that have Mild Cognitive Impairment (MCI) or more severe cognitive impairment, our complete Brain Health Optimization (BHO) Evaluation Program is the suggested starting point. At this point, time is no longer in your favor so the BHOP adds several extensive testing components that allow us to quickly identify the full scope of areas to be addressed.
Note that the BHOP includes all components above plus the additional ones listed below.
Part 1: Baseline Cognitive Assessment including the MoCA and the CNS Vital signs detailed evaluation across 10 domains of cognitive health (eg. memory, executive function, reaction time, cognitive flexibility, etc.)
Part 2: Physical Examination (usually on same day as Part 1)
Part 3: First of 2 x 2hr comprehensive appointments with Dr. Lawson. Day 1 is mostly focused on understanding test results and how they are contributing to the present state of the patient.
Part 4: Second of 2 x 2 hr with your Bredesen-Protocol doctor. This appointment can be in office or it can be a tele-video visit to cover the remaining tests that were not covered in the initial visit and review the core elements of a personalized treatment plan. In this visit, we will present the results of our evaluation in a personalized “cognoscopy”. We are sure that it will be enlightening.
Below is a detailed listing of the dementia/AD tests that are potentially included in the Comprehensive Brain Health Assessment. Note that both programs assume that patient has insurance to cover the baseline labs typically available at Quest/Labcorp under direct insurance billing. Of the remaining listed labs, the $3475 fee includes $1700 that goes towards labs in points 5, 6,7,8,9 and 10 below only. If the patient does not have insurance coverage for the baseline labs, Apollo Health offers the Baseline labs for the cash price of $780 — no insurance required.
- Comprehensive Initial Brain Health Assessment ($3475.00) Includes the following.
- Baseline labs and physical examination. A very complete set of baseline labs that will evaluate the entire spectrum of health and a baseline physical examination closely following the Bredesen protocol. This goes well beyond standard labs to include magnesium, zine and selenium levels, B6, B12 and folate levels, Omega 3 and omega 6 fatty acid levels, pre-diabetes evaluation, hormone levels, thyroid levels as well as specific immune markers like TH1, TH2, IL6 and TNF. These labs are billed to your insurance.
- A baseline Cognitive Assessment. This is to establish a baseline and evaluate you against an age-specific norm to determine the state of your cognitive function today. We are using the CNS Vital Signs cognitive assessment, one of the most highly regarded assessments in the industry.
- Apolipoprotein E (APOE) genetic test. This test is generally not covered by insurance but is an important component to our assessment.
- Biotoxin illness Assessment. As there is emerging data to show that the presence of biotoxin illnesses greatly enhances a patient’s risk for developing AZ, this has to be a part of our brain health assessment. If indicated by a screening questionnaire, the panel leverages the most critical markers from the published literature for determining if a patient’s health is being impacted by CIRS including TGB-Beta 1, MSH, MMP9, HLA DRB1, 3,5, HLA DQB1, ADH/OS and several others. These labs are billed to your insurance.
- Comprehensive infection Assessment. If indicated by a screening questionnaire, the area of assessment and possible testing looks for borrelia, most Lyme coinfections including babesia, bartonella, ehrlichia, Anaplasma phagocytophilum, Chlamydophila pneumoniae and Rocky Mountain Spotted PCR Fever. These labs are billed to your insurance.
- Chemical and heavy metals Immune Reactivity Screen. This area of testing looks for chronic and acute reactivity and antibodies across multiple chemicals and metals including aflatoxins, formaldehyde, bisphenol A, tetrachloroethylene, parabens, mercury, nickel, cobalt, cadmium, lead, arsenic. Potentially Included in Comprehensive Brain Health Assessment fee.
- Urine mycotoxin testing. Looks for presence of key mycotoxins in the urine. Mycotoxins are typically produced by mold exposure but there are other producers of mycotoxins as well. Potentially included in Comprehensive Brain Health Assessment fee.
- Microbiome testing. The gut microbiome resides in your large intestine and is host to more than 1000 species of bacteria that perform certain important functions from shaping the immune system to influencing metabolism of nutrients to fortifying the intestinal mucosal barrier. Microbiome testing helps to identify imbalances in the gut microbiome that may be causing gastrointestinal symptoms, skin conditions, autoimmune disorders, immune system imbalances, and multiple inflammatory disorders. Potentially included in Comprehensive Brain Health Assessment fee.
- Blood brain barrier testing. This test is used to evaluate breaches of the Blood-Brain Barrier by stress, trauma or environmental triggers. Potentially included in Comprehensive Brain Health Assessment fee.
- Inflammation/Immune/Auto-Immune Specialty Genetic Panel. This panel includes 30 gene variants that can affect one’s ability to control/ “turn off” inflammation. Chronic inflammation and oxidative stress can cause premature aging and most chronic diseases, including cancer and is a significant contributor to AD. Understanding a person’s genetic is valuable in both prevention and treatment. Potentially included in Comprehensive Brain Health Assessment fee.
- MRI with Neuroquant (NQ). Listed here for completeness. Not included in the price as this test is covered by most insurances. Used to assess the brain for structural issues and the NQ is used to determine if atrophy or hypertrophy has occurred in the various brain sectors. This is useful for assessing biotoxin illness as well as for broader use in AZ risk. This test is billed to insurance.
- Your own personalized “Cognoscopy”. The Cognoscopy is a summary report that brings together our findings from all of the testing mentioned above and summarizes your risks as it relates to each of the six Alzheimer’s types, and a summary clinical Alzheimer’s disease treatment plan to optimize health and reverse mild cognitive decline if it has begun. Note that to get the actual prescriptions and clinical plan fine details, you must enroll in the Brain Health Optimization Program outlined below.
- Brain Health Optimization Program (BHOP) ($2975 – $9975 for 12 months depending on patient case specifics and scope of our services). Once the evaluation is complete, whether it be the Baseline or Complete program as described above the treatment component begins for those patients that elect to move forward with treatment. Note, prices listed above do not include any medications or supplements. Further, note that all patients who enroll in our Brain Health Optimization Program must commit to a one-year “ReCODE” subscription at $75 per month with Dr. Bredesen and Apollo Health at https://apollo.ahnphealth.com/logins/new. The BHOP includes all of the following to optimize the probability of success:
- Specific and individually tailored lifestyle modification guidance. Through this program component, we will provide specific and tailored guidance to apply all of the lifestyle modifications that we are currently aware of that help to mitigate risk for developing AD. Naturally, this area will continue to emerge so it will be very dynamic as more emerging credible data is published.
- Bioidentical Hormone Replacement as indicated by test results
- Treatment for biotoxin and other chronic illnesses as indicated by test results
- Development and adjustment as needed of a comprehensive clinical plan for the patient that is driven by the ReCode recommendations
- Specific recommended nutritional supplements to enhance brain health.
- All followup visits are included in the program. The number and frequency will vary but expect followup visits (physical or remote) every two weeks in the early part of the program and every 2-3 weeks in the later part of the program.
- Followup Cognitive Assessments 6 months after program commencement and 11 months. We will compare the results of this assessment with the baseline to determine improvement and/or degradation in cognitive function.
Already have labs and your Recode report and just need a physician to review your Recode report and advise of recommended next steps? For this, our Bredesen Recode Report Consultation is the place to start. The fee for this is $1475.00 including a 2.5-hour physician review and consultation.
We are truly excited to bring this program forth to our patient population. Dr. Lawson is passionate about this area of our health and she is committed to being on the leading-edge or the emerging Bredesen treatment protocols. Ready to get started? Use one of the options below.
- Click here to contact us on our quick contact form and someone will get back with you shortly.
- If between the hours of 9:00 AM – 5:00 PM Monday through Friday, feel free to call us now on (703) 822-5003 Ext 2 and our Clinical Intake Coordinator will answer any question you have and get you started.
- If you know this is the program for you, then Click here to begin the online enrollment process
Not ready to start for sure, but just want to get a 30 minute age-normalized cognitive assessment, MoCA evaluation with 30 minute clinical review for $500, then Click here to learn more about our quick but comprehensive neurocognitive assessment.
Helpful Resources for Alzheimer’s disease treatment and the Bredesen Protocol
Here is the proof that the Bredesen Protocol really works. Over 100 patients, multiple practitioners, multiple geographies, results sustained over time. Click here to read the details:
Check out this report that concludes why existing drugs and drugs that once showed promise in early clinical trials have failed. Bottom line, Dr. Bredesen and the ReCode protocol has the answers. Traditional therapies are stuck looking for the “magic bullet”. Click here to read more…
Think mold exposure can’t be the cause of your cognitive decline, read what Dr. Amen of the world renowned Amen Clinics has to say about the subject. Click here to read Dr. Amen’s thoughts.
This book is a must read for patients suffering from dementia/Alzheimer’s disease and are searching for effective dementia treatment. “You can fix your brain: Just 1 hour to the best memory, productivity, and sleep you’ve ever had”. Get it at Amazon here. http://Just 1 Hour a Wek to the Best Memory, Productivity, and Sleep You’ve Ever Had

